An 11-month-old German Shepherd cross was recently the focus of a considerable amount of neurological inpatient rehabilitation at SCVS after having undergone neuro-orthopaedic surgery to stabilise a high level C1-C2 vertebral fracture with an autogenous cancellous bone graft and two bridging reconstruction plates. The dog presented to the inpatient physiotherapy team with bilateral flaccid paralysis of the forelimbs and significant paraparesis of both hind limbs. Head and neck control was poor and the dog was unable to maintain any functional postural sets including sternal recumbency due a substantial lack of abdominal core stability and control.
Initial therapeutic input focused on assisting with pain control and joint range of movement via the use of soft tissue massage and passive joint exercises, techniques that in human physiotherapy have been shown to be clinically very effective at preserving and maintain upper limb function in stroke patients admitted to an ICU setting (Kim et al 2014).
Once the dog’s overall condition had stabilised, rehabilitation switched focus onto task specific training, a concept based on the theory of neuroplasticity and incorporates exercises designed to stimulate the proprioceptive and sensory feedback mechanisms considered key in facilitating and re-establishing specific aspects of locomotor spinal circuitry (Hubli and Dietz 2013).
His first active session consisted of an assisted standing exercise using a peanut roll in order to maintain his body weight. This initial exercise was chosen as a means of trying to increase muscle tone by stimulating afferent feedback mechanisms via limb loading, a model of treatment also supported in human neurological studies (Harkema et al 1997).
After 2 weeks of intensive inpatient rehabilitation, the patient was starting to show significant improvements in hind limb activity and was beginning to weight bear using his back legs when supported in a harness. His forelimb function was slower to resolve, with his right forelimb still significantly dragging on assisted walking. Head and neck control was still reduced with the dog using broad movements to move his head to either side.

Physiotherapist encouraging Tyson to perform sit to stand.
Further therapy started to focus on the use of functional postural sets in order to continually improve muscle tone whilst facilitating normal limb alignment and head neck position. Appropriate positioning of the limbs whilst in sitting and utilising techniques such as rhythmical stabilisations help to improve a neurologically compromised dog’s initial core stability and static balance. By the end of the 3rd week, the dog was able to start changing his own recumbent position with very little assistance.
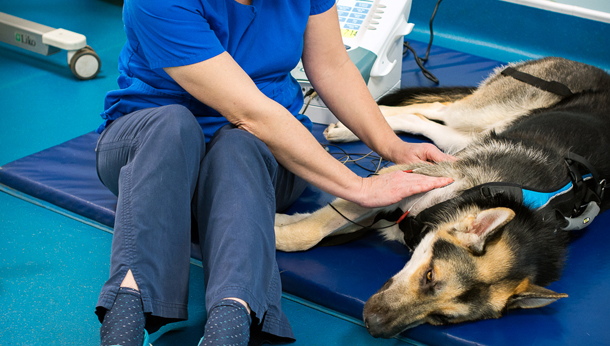
Physiotherapist performing muscle stimulation on Tyson.
In order to prevent atrophy of the right forelimb, neuromuscular electrical nerve stimulation was employed to the muscle groups of the right shoulder and the effects of this were immediately apparent as the dog started to try and place the limb appropriately when walked back to the ward area.

Tyson in the under-water treadmill.
Consistent input and the start of hydrotherapy via the daily use of the under water treadmill saw the dog’s mobility and function significantly improve over following two weeks. He was able to ambulate using all 4 limbs in an appropriate gait pattern, although assistance with 2 people was still required as he remained deconditioned overall. His ability to carry out independent transfers markedly improved and he showed signs of attempting to sit to stand without assistance.
After 5 weeks of consistent inpatient physiotherapy, the dog was sent home with a home exercise plan designed to build upon his initial improvements. Assisted sit to stand exercises, weight sways in standing and alternate legs lifts were detailed to the owner. He is now seen as an out-patient for further rehabilitation and progression of his mobility and he continues to make strides towards the goal of a full and enjoyable active lifestyle.
For more information on our physiotherapy service click here.
References:
Harkemma, S.J., Hurley, S.L., Patel, U.K. (1997) Human lumbosacral spinal cord interprets loading during stepping. Journal of Neurophysiology. 77, pp. 797-811.
Hubli, M. and Dietz, V. (2013) The physiological basis of neurorehabilitation – locomotor training after spinal cord injury. Journal of Neuroengineering and Rehabilitation. 10 (5), pp. 1-8
Kim, H.J., Lee, Y. and Sohng, K, Y. (2014) Effects of bilateral passive range of motion exercise on the function of upper extremities and activities of daily living in patients with acute stroke. Journal of Physical Therapy Science. 26, pp. 149-156.