Nacho, a six year old male French bulldog, was referred to SCVS for further investigation of acute onset left-sided facial swelling.
Ten days previously Nacho had been presented to his referring practice with nystagmus and given his history of otitis externa, vestibular dysfunction associated with otitis media and interna were suspected. A head tilt was noted three days later and the left ear canal was cultured and flushed. Four days after the ear flush, Nacho returned to his local practice due to vomiting, inappetence and lethargy. Whilst Nacho generally improved with supportive treatment, he then developed swelling on the left side of his face which quickly worsened.
When Nacho was presented to SCVS the clients felt that the swelling had reduced. On examination Nacho was extremely depressed and the left globe could not be retropulsed to the same extent as the right. Anisocoria was present with left pupillary miosis. Nacho was unable to blink on the left side consistent with facial nerve dysfunction. Chemosis, episcleral injection and third eyelid protrusion were evident in the left eye. A mild head tilt (left side down) was present.

3D volume rendered reconstruction.
A CBC and serum biochemistry profile revealed a neutrophilia but no other abnormalities of concern. On CT, soft-tissue attenuating material was visible in both tympanic cavities along with bulla wall thickening, consistent with bilateral otitis media. Soft tissue-attenuating material was also visible filling the horizontal ear canals and the walls of the canals were mineralised in places. The left zygomatic salivary gland was enlarged and heterogenous in appearance. The right zygomatic salivary gland was considered normal in size but also had a heterogenous appearance. The enlarged left zygomatic salivary gland was herniating rostrally, ventral to the left orbit and over the dorsolateral aspect of the zygomatic arch. Under the same anaesthetic, a swab for culture was taken from the left ear canal and this ear canal was flushed again as it was filled with pus. A central area of fluorescein uptake on the left cornea indicated corneal ulceration. Aspirates of the left zygomatic salivary gland were poorly cellular but the cell population predominantly comprised non-degenerate neutrophils with rare mesenchymal cells.
The main differentials for the salivary gland enlargement were sialadenosis and sialadenitis with a definitive diagnosis requiring histopathology. Due to a postulated link between oesophageal/gastrointestinal disease and sialadenitis Nacho was started on a metoclopramide infusion and omeprazole. As a response has been reported in cases of sialadenosis and sialadenitis to phenobarbital this was also started in addition to i/v fluids, analgesics and antibiotics. Nacho ate overnight and was much brighter the following morning but later that day regurgitated twice, wouldn’t eat and acutely developed marked right-sided facial swelling with concurrent pyrexia.
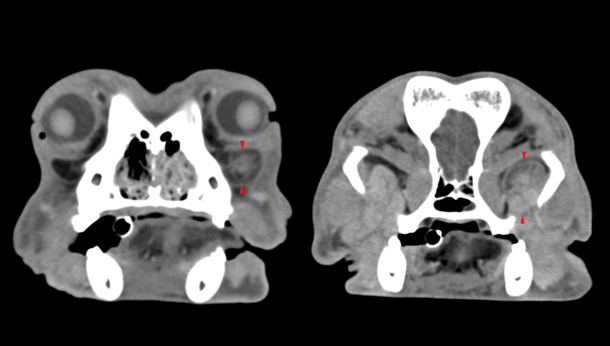
Transverse images of the head showing enlargement and heterogenous appearance of the left zygomatic salivary gland (between arrow heads).
Over the next 48 hours, the right sided facial swelling steadily reduced and no further regurgitation occurred. The left episcleral injection and chemosis also improved. Swelling remained palpable immediately ventral to the left orbit consistent with the location of the enlarged and herniated left zygomatic salivary gland on the CT. The swelling on the right side was in a slightly different position, as though the zygomatic salivary gland was herniating ventral to the zygomatic arch, and was most easily appreciated by feeling along the buccal aspect of the upper right dental arcade. A repeat CT to confirm suspected enlargement of the right zygomatic salivary gland and biopsy to obtain samples for histopathology were discussed with the clients, however given that the left salivary gland swelling had started to regress quite quickly we decided to monitor his progress for a few days rather than proceed with a second anaesthetic.
Nacho was discharged at this stage and follow-up care for his corneal ulcer was kindly performed by his referring practice. When the clients returned Nacho to SCVS for a check-up one week later they reported they had witnessed no further regurgitation and that Nacho had regained a keen appetite including crunching biscuits and biting his toys which he had previously been hesitant to do. They reported that he continued to have balance issues, for example staggering or falling over if he shook his head. Examination at this stage revealed resolution of the facial swelling bilaterally and the left cornea no longer took up fluorescein. The episcleral injection had resolved but the left sided facial nerve dysfunction persisted. At this stage the presumed sialadenosis/-itis appeared to have resolved and I suspected the residual clinical signs were attributable to otitis. Following discussion with the clients and Nacho’s dermatologist Paul Coward we elected to proceed with a left TECA/LBO surgery.
At a re-check appointment four weeks post-surgery the clients reported that Nacho was doing very well – no longer falling over when he shook and with a much more coordinated gait. A mild head tilt remained visible and he remained unable to blink the left eyelids. As there had been no clinical signs of salivary gland swelling for over six weeks I advised slowly tapering the phenobarbitone course.
I spoke to the clients this week for an update – it is now five months since the TECA/LBO surgery and two months since the cessation of phenobarbitone. They reported that their referring vet has confirmed that Nacho has regained the ability to blink, no longer has a visible head tilt and has no residual balance problems. There has been no recurrence of the facial swelling and no clinical signs related to the right ear.
Nacho was an intriguing case as well as being a charming patient – his high-pitched bark sounds very much like a person saying “help” and on more than one occasion he caused staff to come rushing to the ward to see who needed help!
Nacho’s presentation was somewhat confusing due to there being, with hindsight, three conditions (presumed sialadenosis/-itis, otitis and corneal ulceration) that are not all obviously linked. I suspect the corneal ulcer was the result of facial nerve dysfunction (inability to blink) or due to damage to the parasympathetic fibres carried in the chorda tympani in the tympanic cavity leading to reduced tear secretion. The facial nerve dysfunction and Horner syndrome were likely to be the result of the otitis media. The head tilt and vestibular signs suggest a progression to otitis interna. At a stretch it seems possible that innervation to the salivary glands could have been affected if the tympanic nerves/plexuses were damaged but it is unknown whether this could explain the salivary gland swelling. Dysfunction of the innervation of the salivary glands has been proposed as the aetiology for human sialadenosis.
We are very grateful to Aniwell Veterinary Clinic, in particular vets Bruce and Caroline, for referring this case and for their care of Nacho following his visits to SCVS. We would also like to thank Paul Coward for his cooperation and advice.